The American Gastroenterological Association recently published a guideline on the management of pouchitis and inflammatory pouch disorders (Gastroenterology 2024;166[1]:59-85). GEN’s Sarah Tilyou spoke with lead author Edward Barnes, MD, MPH, an IBD specialist and assistant professor of medicine at the University of North Carolina at Chapel Hill, about the new guideline and its implications for practice.
GEN: What prompted the guideline?
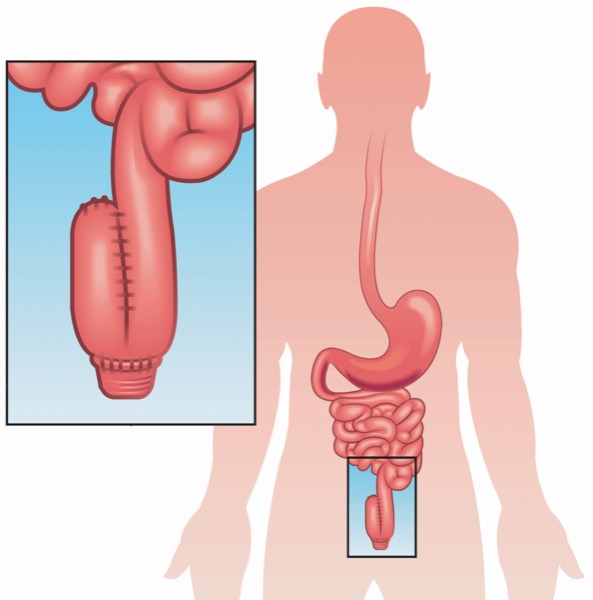
Dr. Barnes: This is the first society-sponsored guideline related to pouchitis and inflammatory conditions of the pouch. There’s been a push in the last five or 10 years to standardize our approach and delve into the evidence on treating patients after they undergo an ileal pouch–anal anastomosis (IPAA) surgery and have these inflammatory conditions in the pouch. There have been several different consensus statements and different research groups that have led this push to standardize, but now we have come together as a group to develop consensus definitions on what these inflammatory conditions are, what the state of the evidence is and what the future directions are.
GEN: What’s new in the guideline that clinicians need to know?
Dr. Barnes: There are a couple of important points that are new and that codify what we have known for a long time. I separate those into two areas.
One is that we were very deliberate in how we tried to define these inflammatory conditions of the pouch. There is some new terminology, for example, the idea of intermittent pouchitis, which is really the most common complication after IPAA. In the literature, for a long time, this has been referred to as acute pouchitis. But it has been difficult to determine what acute pouchitis is and when that patient starts to transition to chronic pouchitis. Patients often have intermittent episodes of pouchitis, in which they have a defined increased activity that’s presumably related to inflammation in their pouch, but when we treat them with antibiotics or some other therapy, they undergo long periods of normal pouch function without additional therapy. We chose the term intermittent pouchitis for this, moving away from the less accurate term acute pouchitis.
The second thing we tried to do is better define chronic pouchitis. We wanted to get away from numeric definitions of more than four episodes per year, which has been the traditional definition in the literature. Some patients who are treated with antibiotics have recurrence of symptoms once the antibiotics are stopped. The condition is not intermittent anymore in these patients. They really need antibiotics all the time and would be considered to have chronic antibiotic-dependent pouchitis. In some patients—those with chronic antibiotic-refractory pouchitis—antibiotics stop working, and we start thinking about using immunosuppressive therapies and advanced therapies such as biologics and small molecules.
Those definitions, plus the definition of Crohn’s-like disease of the pouch, a term that has been used over the past several years, are some things that were new.
Another new idea we discussed was when the appropriate time is to introduce advanced therapies for patients with chronic pouchitis. That was informed by some really interesting discussions the guideline panel had, as well as by the landmark EARNEST trial published last year, which evaluated vedolizumab [Entyvio, Takeda] in the treatment of chronic pouchitis [N Engl J Med 2023;388(13):1191-1200]. In the trial, investigators treated patients with antibiotics at the time of enrollment, then gave them vedolizumab or placebo. Vedolizumab was associated with improved remission rates in these patients with chronic pouchitis after IPAA. We are trying to get at the idea of whether we should be treating patients with chronic pouchitis earlier with advanced therapies, whether there is a potential advantage of that if a patient doesn’t want to take chronic antibiotics, with shared decision making between the treating provider and the patient.
GEN: Is there pushback from payors on use of biologics for patients with pouchitis?
Dr. Barnes: One thing that we are always cognizant of is how do we get patients appropriate access to medicines when they need them, and in the United States, insurance companies are a big piece of that puzzle. Although patients no longer technically meet a definition of ulcerative colitis after they have surgery and an IPAA because they don’t have a colon anymore, they still have the underlying IBD phenotype. I think that’s important for us as treating providers to remember, and it’s also important for the insurance companies to remember. That underlying phenotype that made that patient have such bad ulcerative colitis that they didn’t respond to available treatments and required surgery is still there. Some of these patients develop these chronic inflammatory conditions after surgery and will need reintroduction of these advanced therapies. We tried to be cognizant of that when we talked about what therapies potentially could be useful in that scenario.
Although no advanced therapies are specifically approved for pouchitis, current evidence indicates that anything that’s been approved for ulcerative colitis or Crohn’s disease conceivably could be used in that situation. We don’t have large randomized controlled trials or head-to-head comparative effectiveness studies outside of the EARNEST study and one small study of adalimumab. So we’re really trying to make these decisions on a one-on-one basis, considering a patient’s individual characteristics. Sometimes we do have pushback from insurance companies, but in the guidelines we aimed to help treating providers avoid some of this pushback in the future, so we can get these effective therapies to patients earlier.
GEN: How might the guideline change practice?
Dr. Barnes: I think a couple of different ways. One is that for a long time, there have been gray areas in how we treat pouchitis and inflammatory conditions of the pouch to some degree, and if you weren’t practicing in major academic IBD centers, you didn’t see a lot of patients with pouchitis and inflammatory conditions of the pouch. When I would talk to treating providers, they would have a lot of questions about pouchitis and did not have a sense of comfort with how they were taking care of patients in this scenario. The biggest thing we are trying to do is minimize these gray areas where people have all these questions and help clinicians guide their management approach from the beginning according to the available evidence.
GEN: What were some of the hottest points of debate among the guideline panel, and how did you resolve them?
Dr. Barnes: One topic about which there was a little bit of a debate, and that has generated a lot of questions from patients for years, relates to the role of probiotic therapy in both the prevention and the treatment of pouch-related disorders. This has been covered to some degree by prior AGA guidelines, although they were focused on probiotics and probiotic therapy, not on pouchitis.
One reason this has generated a lot of discussion is that the evidence for the use of probiotics, particularly in the area of primary prevention, and even in secondary prevention, is relatively robust. There are some randomized controlled trials, and they showed a pretty big delta when you compare those probiotic therapies versus placebo. What is sort of lacking there is the translation into the real world. Even in some of the real-world studies where they’ve used the same formulations or the same probiotics, patients haven’t had the same effect. That generated a lot of discussion among the guideline panelists regarding weighing real-world evidence versus what we know from a few small randomized controlled trials.
The second thing that also generated a lot of discussion was the role of endoscopic evaluation, or specifically a pouchoscopy, among patients with a suspected inflammatory condition in the pouch. For a long time, people would say if you suspect that a patient has pouchitis, you need to do a pouchoscopy to confirm that before you treat them with antibiotics. I don’t disagree that it would be nice to confirm in every patient that their symptoms are being driven by active inflammation of the pouch. But we know a couple of things. One is that clinical symptoms don’t always track with the degree of inflammation that you see on pouchoscopy. And we also know that, logistically, in terms of practice patterns in the United States across most centers, if a patient calls you and says, “I have increased frequency” or “I have abdominal pain” or “I’m having unusual nighttime stools that are waking me up,” it’s difficult to say, “Come in and we’ll do a pouchoscopy tomorrow morning.” That’s just not how most practices function. But we can write a prescription for antibiotics, and in most cases, their symptoms are going to get better within 24 to 48 hours.
So, as a guideline panel, we said endoscopy is not necessary for every first episode of pouchitis. But if a patient is having recurring symptoms, or you have a reason to suspect that something else is going on, certainly you should be following that up with a pouchoscopy to make sure that you understand exactly what’s driving that patient’s symptoms.
GEN: What are the biggest gaps in evidence remaining in this area?
Dr. Barnes: I think one big gap is to determine who’s at risk for pouchitis and the role of prevention. There is an opportunity for earlier intervention that is fueled in some ways by some of what I mentioned before about probiotics. We made a recommendation that secondary prevention could be considered in patients who are interested in taking probiotics. The other reason I mention prevention is that there’s a suggestion that the incidence rate of pouchitis may be increasing. We still don’t know who is at the highest risk for pouchitis outside of those with some classic predictors, such as primary sclerosing cholangitis. Better defining the high-risk groups, by either clinical or translational approaches—that’s a big gap that needs to be filled.
A second big gap is that we still need better study design and a better evidence base when we think about determining how to best treat patients after they develop these inflammatory conditions of the pouch. I mentioned the landmark EARNEST study, which is a randomized controlled trial. I don’t think every single study for every potential therapy to treat patients with a pouch needs to be a randomized controlled trial. We can consider comparative effectiveness studies, pragmatic clinical trials, and don’t necessarily need a placebo control in every trial. We probably need to think a little bit outside the box in terms of our study design. Another approach is large prospective registries. I’m a little bit biased because that’s the kind of research that we’ve been doing at UNC. With these multicenter registries, we probably will be able to more quickly answer some of these questions.
GEN: Is there any other take-home message that you want to end with to wrap up?
Dr. Barnes: It was very exciting to be a part of the first set of society guidelines and going through the evidence base supporting management of patients with pouchitis. But perhaps just as exciting was the opportunity to really codify and try to standardize and spell out an approach to managing these patients. This is not the one end-all, be-all; we’re going to continue to reevaluate the new evidence and incorporate that into future guidelines, but I hope that treating clinicians find this first iteration valuable to fill in some of the gaps.
This article is from the July 2024 print issue.