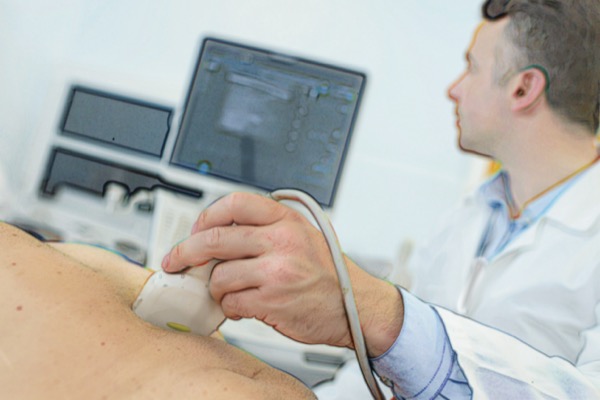
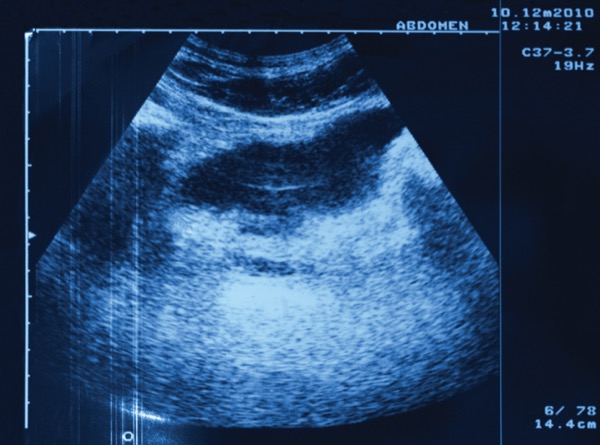
LAS VEGAS—Managing inflammatory bowel disease with intestinal ultrasound could lead to a significant improvement in patient outcomes, according to a presentation at the 2024 Crohn’s & Colitis Congress.
“Every IBD patient that walks through the door should have access to intestinal ultrasound,” according to Noa Krugliak Cleveland, MD, the director of the Intestinal Ultrasound Program at the University of Chicago Medicine’s Inflammatory Bowel Disease Center. “Whether the patient has ulcerative colitis, Crohn’s disease, a J pouch or perianal disease, this procedure expedites treatment decision making and can replace other invasive tools. We believe it will also transform clinical outcomes.”
While “traditional monitoring strategies are invasive, require extensive preparation, often are not well tolerated by patients, and do not provide real-time results,” IUS is a point-of-care test that can be completed during a clinic visit, Dr. Krugliak Cleveland said.
The number of gastroenterologists who perform IUS in the United States is growing, she noted, and the procedure has been well received and is preferred by patients. A recent survey of pediatric patients and their caregivers found high satisfaction with the use of transabdominal bowel ultrasound, which was preferred to colonoscopy, sigmoidoscopy, stool sampling and blood tests for IBD assessment (J Pediatr Gastroenterol Nutr 2023;76[1]:33-37).
“Patients felt that ultrasound helped them to know more about their disease, where their symptoms came from and make more informed decisions about managing their IBD,” Dr. Krugliak Cleveland said.
Accurate Diagnostics And Disease Monitoring
Intestinal ultrasound compares favorably to endoscopy or commonly used endoscopic indices. In fact, Dr. Krugliak Cleveland said, studies show that IUS correlates with endoscopy better than the Harvey-Bradshaw Index, C-reactive protein or fecal calprotectin (J Crohns Colitis 2021;15[1]:115-124; Clin Gastroenterol Hepatol 2022;20[4]:e723-e740; United European Gastroenterol J 2022;10[2]:225-232).
Furthermore, IUS and magnetic resonance elastography (MRE) have comparable diagnostic accuracy for small bowel disease activity. In the METRIC trial—the largest prospective, multicenter comparison trial of IUS and MRE, which included 284 IBD patients—the sensitivity for terminal ileum disease was 97% for MRE and 92% for IUS (Lancet Gastroenterol Hepatol 2018;3[8]:548-558).
According to Dr. Krugliak Cleveland, IUS enables tight disease monitoring and assessment of transmural healing. The STRIDE-II systematic review, which encompasses evidence- and consensus-based recommendations for treat-to-target strategies in adults and children with IBD, suggested that sonographic transmural healing is a future therapeutic target and that “the use of bedside ultrasound has revolutionized our ability to assess the degree of inflammation in IBD” (Gastroenterology 2021;160[5]:1570-1583).
An analysis of one-year clinical outcomes with biologics in Crohn’s disease also indicated that sonographic transmural healing may be a superior outcome to endoscopic mucosal healing (Aliment Pharmacol Ther 2019;49[8]:1026-1039). Sonographic transmural healing was associated with higher rates of steroid-free clinical remission, lower rates of clinical relapse, and a lower need for hospitalization or surgery—even after discontinuation of biologics.
Furthermore, IUS has been shown to shorten time-to-treatment change and time to clinical remission. In an analysis of data on 105 patients treated with an eight-week upadacitinib (Rinvoq, AbbVie) induction, Dr. Krugliak Cleveland and her co-investigators found an average time-to-treatment change of 1.1 days for patients receiving ultrasound versus 16.6 days for conventionally managed patients (American College of Gastroenterology 2023 plenary 36). The average time to clinical remission was 26.8 days in the IUS group versus 55.3 days in the conventional management group. What was important, she said, is that this study matched patients by providers and disease phenotype.
Finally, Dr. Krugliak Cleveland underscored the potential cost savings of this approach. The billing codes that are already in place for IUS generate an estimated revenue of $800 per exam, said Dr. Krugliak Cleveland, noting that “approximately 50 exams will pay for a midrange ultrasound machine.”
High Sensitivity And Specificity
Lee A. Denson, MD, the director of the Schubert-Martin Inflammatory Bowel Disease Center and a professor at Cincinnati Children’s Hospital Medical Center, called the journey of IUS from radiologists to GIs to radiologists to GIs again “fascinating to watch over the past 30 years.”
Commenting on Dr. Krugliak Cleveland’s presentation, he said one potential limitation of IUS is examination of thick segments of the terminal ileum or sigmoid colon.
“In parts of the small bowel where there is going to be a lot of gas in the way, I worry about being falsely reassured [and possibly miss pathology] in the office,” Dr. Denson said.
But Dr. Dr. Krugliak Cleveland countered that “actually, the negative predictive value of intestinal ultrasound is very high, with sensitivity and specificity of IUS of 89% and 94.3%, respectively” [Inflamm Bowel Dis 2016;22(5):1168-1183]. “So, if you don’t see inflammation in a Crohn’s patient, you have high certainty that there is no active disease. Although air used to be a huge consideration, with current ultrasound image resolution and graded compression by the sonographer, you can see all of the bowel wall to submillimeter resolution.”
—Chase Doyle
Dr. Denson reported no relevant financial disclosures. Dr. Krugliak Cleveland reported financial relationships with BMS, NeuroLogica (a subsidiary of Samsung) and Takeda.
This article is from the March 2024 print issue.