Patients with Clostridioides difficile infections who also have metabolic dysfunction–associated steatohepatitis are at increased risk for death and other severe complications, according to a retrospective study drawn from the National Inpatient Sample.
The investigators, from Rutgers-Robert Wood Johnson Medical School, in New Brunswick, N.J., noted that there is evidence that metabolic-dysfunction–associated steatotic liver disease (MASLD) or metabolic-dysfunction–associated steatohepatitis (MASH) can lead to inflammation and increased infection risk, possibly as a result of impaired function of liver macrophages, which are the first immune cells to process antigens and pathogens in the gastrointestinal tract. Gut microbiome alterations in MASLD or MASH also may contribute to greater risk for C. difficile infection (CDI) and severity.
The study included records from 745,475 patients with a diagnosis of CDI only, 4,366 with a diagnosis of MASH and CDI, and 11,335 with a diagnosis of MASLD and CDI between 2015 and 2017. The patients’ mean age was 66 years and 42.42% were female.
The researchers found that patients with CDI and MASH had a higher mean Charlson Comorbidity Index score (6.33) than patients with CDI only (5.12) or CDI and MASLD (3.40) (P<0.001). Mortality was higher in the CDI plus MASH cohort, at 7.11%, versus 2.1% for CDI plus MASLD and 6.36% for CDI alone.
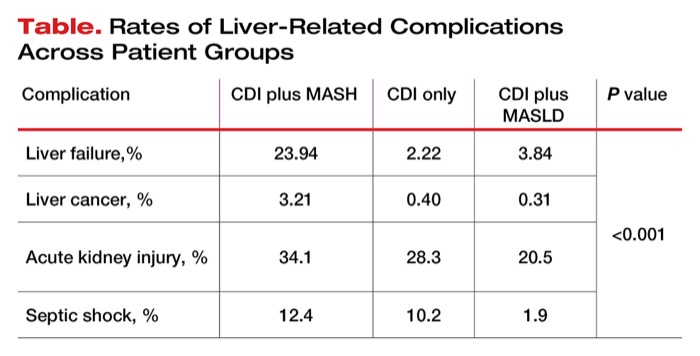
Liver-related complications also were higher in the CDI plus MASH group than in those with CDI only and MASLD plus CDI (Table).
| Table. Rates of Liver-Related Complications Across Patient Groups | ||||
| Complication | CDI plus MASH | CDI only | CDI plus MASLD | P value |
| Liver failure,% | 23.94 | 2.22 | 3.84 | <0.001 |
| Liver cancer, % | 3.21 | 0.40 | 0.31 | |
| Acute kidney injury, % | 34.1 | 28.3 | 20.5 | |
| Septic shock, % | 12.4 | 10.2 | 1.9 | |
Some ‘Holes’ in the Data
Commenting on the findings in an interview with GEN Priority Report, Sahil Khanna, MBBS, expressed some surprise at the lower mortality risk among patients with MASLD plus CDI than those with CDI. “I don’t know if I can make biological sense out of it,” said Dr. Khanna, who leads the clinical and research program at Mayo Clinic in Rochester, Minn., involving fecal microbiota transplantation for CDI.
Noting that the study did not control for comorbid conditions, Dr. Khanna said, “I think there’s a lot of holes in this data before we start telling people that if you get C. difficile in the hospital, you’re twice as likely to die if you have [MASLD].”
Manal Abdelmalek, MD, who also was asked to comment on the study, said the investigators used ICD-10 codes, which may not accurately stratify MASLD from MASH or define the severity of underlying liver disease. But she acknowledged that patients with fatty liver disease and particularly those with advanced hepatic fibrosis and cirrhosis are at increased risk for infections and poor clinical outcomes related to bacterial infections. “It is unclear whether the increased mortality in patients with C. difficile and [MASH] is attributable to the presence of chronic liver disease or associated complications of metabolic syndrome.”
In particular, diabetes is a source of concern, according to Dr. Abdelmalek, the director of the NAFLD Clinical Research Program at Mayo Clinic in Rochester. “The prevalence of [MASH] among patients with type 2 diabetes is more than twofold higher than in the general population. Diabetes mellitus is a strong predictor for hepatic fibrosis in patients with [MASH]. In this analysis, we don’t know if diabetes was a confounding factor. Patients with diabetes may have slower gastrointestinal motility; impaired wound healing response; and they may have hyperglycemia, which can increase morbidity and mortality from C. difficile and other bacterial infections,” she said.
However, Dr. Khanna said if the study’s findings are confirmed, they would further underline the need to manage MASLD to reduce hepatitis.
Just as important as identifying CDI in patients with MASH, Dr. Abdelmalek stressed that when a physician has a C. difficile patient with metabolic risk factors, “it’s very important … to consider the potential for underlying [MASH] and risk-stratify with noninvasive tools to define the presence or absence of advanced hepatic fibrosis or cirrhosis, because patients with undiagnosed and unrecognized cirrhosis can more readily get into trouble from C. difficile infection. It gets to the issue of early diagnosis and recognition of liver disease, which sometimes falls below the radar screen.” In addition, she said, chronic liver disease and obesity and associated metabolic syndrome are linked to higher use of the healthcare system and heightened hospitalization risk, and, in turn, the potential for higher risk for C. difficile exposure.
—Jim Kling
Dr. Abdelmalek reported a financial relationship with Intercept. Dr. Khanna reported financial relationships with Finch, Immuron, Niche, Pfizer, Probiotech, Rebiotix/Ferring, Seres, Takeda and Vedanta.
This article is from the November 2023 print issue.