FASGE, FACG, FACP, AGAF
Director of Endoscopic Research and Development
The University of Texas MD Anderson Cancer Center
Houston
In this month’s column, I picked three recent studies from the endoscopic ultrasound literature published over the last few months.
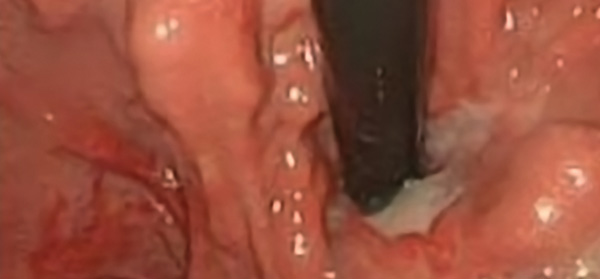
Historically, it has been harder to treat gastric varices endoscopically than esophageal varices. We used to treat esophageal varices with sclerotherapy, and then band ligation revolutionized the treatment of esophageal varices, allowing their obliteration with fewer complications. Subsequently, endoscopic cyanoacrylate (CYA) injection became an option for endoscopic treatment for gastric varices. With the advent of EUS-guided interventions, it has become possible to not only inject CYA precisely but to also place embolization coils into gastric varices. Randomized comparative trials are difficult to do in endoscopy, and the first study I picked is a randomized comparative trial of the safety and efficacy of EUS-guided coil embolization plus CYA injection versus EUS-guided CYA injection alone.
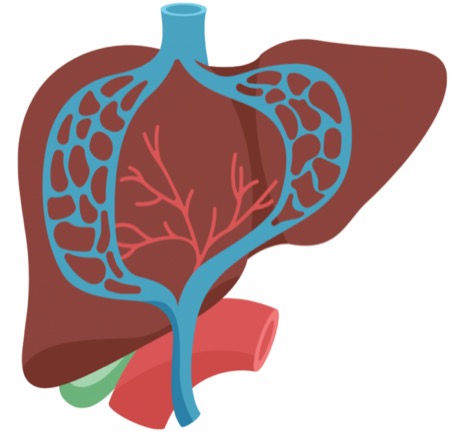
Another recent development in “endohepatology” is the ability to measure portal pressure gradient (PPG) under EUS guidance in a minimally invasive manner. This is an important measure for assessing the severity of and taking care of patients with chronic liver disease. The traditional method to check this is via a transjugular approach to measure the hepatic venous portal gradient (HVPG). Researchers from Spain performed a study comparing these two methods in the same group of patients.
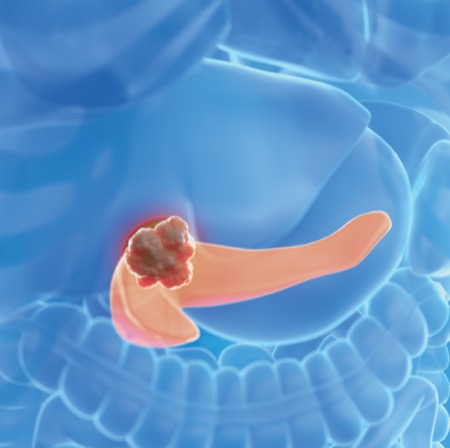
The third study I picked focuses on enhanced EUS imaging with contrast-enhanced EUS (CEH-EUS). There are potentially useful applications of CEH-EUS, such as in differentiating true mural nodules from mucin balls in pancreatic cystic neoplasms. CEH-EUS also has been touted as possibly improving the diagnostic accuracy of EUS-guided tissue acquisition, but in this meta-analysis of published studies, there did not appear to be any benefit of CEH-EUS for EUS-guided tissue acquisition in solid pancreatic masses.
EUS-Guided Coil Embolization and CYA Versus CYA Alone for Gastric Varices
Endoscopy 2024 Sep 18. doi:10.1055/a-2408-6905
Investigators at a tertiary care center in India conducted a randomized trial to compare the safety and efficacy of EUS-guided coil embolization plus CYA injection versus EUS-guided CYA injection alone in patients with gastric varices.
In total, 50 patients were randomized, with 25 in each arm. The clinical success, defined as variceal obliteration, and technical success of each intervention were high; clinical success was achieved in 100% of those in the coil plus CYA arm and 92.3% in the CYA-only arm (P=0.49), and technical success was achieved in all patients in both arms.
During EUS at 12 weeks post-intervention, variceal reappearance was somewhat less common among those in the coil plus CYA arm compared with the CYA-only arm (12.5% vs. 19.2%; P=0.70).
Where the two interventions seemed more clearly differentiated was in the need for reintervention. Among those in the coil plus CYA arm, 20.8% needed reintervention, compared with 53.8% of those in the CYA-only arm (P=0.03). The time to reintervention also was longer in the coil plus CYA arm (P=0.01).
Of note, those in the coil plus CYA arm also had a statistically significant longer survival than those in the CYA-only arm (P=0.04).
EUS-Guided Portal Pressure Gradient Measurements And Hepatic Venous Pressure Gradient
Endoscopy 2024 Sep 3. doi:10.1055/a-2369-0759
Researchers at a single center in Spain evaluated EUS-guided PPG measurement as an alternate approach to the gold-standard HVPG measurement.
Thirty-three patients who had chronic portal hypertension underwent PPG measurement on two occasions: once with transjugular HVPG and once with EUS-guided PPG using a 22-gauge needle. For each technique, technical success was achieved in 31 patients (93.9%), and in 30 patients, technical success was achieved using both techniques. Among these 30 patients, the PPG measurements were compared.
The correlation of EUS-PPG and HVPG measurements was high, with an intraclass correlation coefficient of 0.82. For four of the 30 patients (13.3%), there was a discrepancy of 5 mm Hg or more between the two measures.
The safety of the two measurement techniques was comparable.
EUS-Guided Tissue Acquisition From Solid Pancreatic Masses
Pancreatology 2024;24(4):649-660
Investigators conducted a systematic review and meta-analysis of studies that compared the utility of CEH-EUS with conventional EUS for tissue acquisition from solid pancreatic masses.
The investigators identified nine relevant randomized and observational studies that compared the two techniques across outcomes of diagnostic adequacy, tissue yield, number of needle passes, rate of technical failure and/or rate of adverse events.
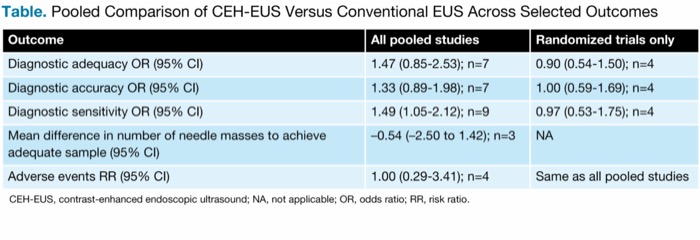
The investigators found no significant differences in the diagnostic adequacy or diagnostic accuracy of the CEH-EUS and conventional EUS methods in their pooled results for all studies or randomized trials only. While there was a significant difference in the diagnostic sensitivity, favoring CEH-EUS, this was driven by the results of non-randomized studies. The investigators noted that they believed these differences were driven by unmeasured or unresolved confounding by baseline factors in these observational studies. Specific measures for selected outcomes are included in the Table.
| Table. Pooled Comparison of CEH-EUS Versus Conventional EUS Across Selected Outcomes | ||
| Outcome | All pooled studies | Randomized trials only |
|---|---|---|
| Diagnostic adequacy OR (95% CI) | 1.47 (0.85-2.53); n=7 | 0.90 (0.54-1.50); n=4 |
| Diagnostic accuracy OR (95% CI) | 1.33 (0.89-1.98); n=7 | 1.00 (0.59-1.69); n=4 |
| Diagnostic sensitivity OR (95% CI) | 1.49 (1.05-2.12); n=9 | 0.97 (0.53-1.75); n=4 |
| Mean difference in number of needle masses to achieve adequate sample (95% CI) | –0.54 | NA |
| Adverse events RR (95% CI) | 1.00 (0.29-3.41); n=4 | Same as all pooled studies |
| CEH-EUS, contrast-enhanced endoscopic ultrasound; NA, not applicable; OR, odds ratio; RR, risk ratio. | ||
While the investigators acknowledged that the level of evidence across studies for the various outcomes ranged from very low to moderate, they concluded there is no evidence for a benefit of CEH-EUS over conventional EUS for improving diagnostic adequacy of pancreatic solid mass tissue sampling.
This article is from the November 2024 print issue.