Patients with cirrhosis who also have primary liver cancer face a higher risk for complications and death when they have portal vein thrombosis (PVT), new research confirms.
The findings highlight the need for early detection and treatment of PVT in these high-risk patients, according to study author David U. Lee, MD, an advanced hepatology fellow at Tufts Medical Center, in Boston, at the time of the study. “This study strengthens the known association between PVT and adverse outcomes in cirrhosis patients with liver cancer using a national registry,” Dr. Lee told Gastroenterology & Endoscopy News. He and his colleagues presented the findings at the 2021 virtual Digestive Disease Week, where the research was named a Poster of Distinction (abstract Su344).
Dr. Lee’s team compared hepatic events, hospital length of stay, hospital costs and mortality between patients with and without PVT, using data from nearly 39,000 patients with cirrhosis and primary liver cancer (hepatocellular carcinoma or cholangiocarcinoma) from the National Inpatient Sample for 2011-2017.
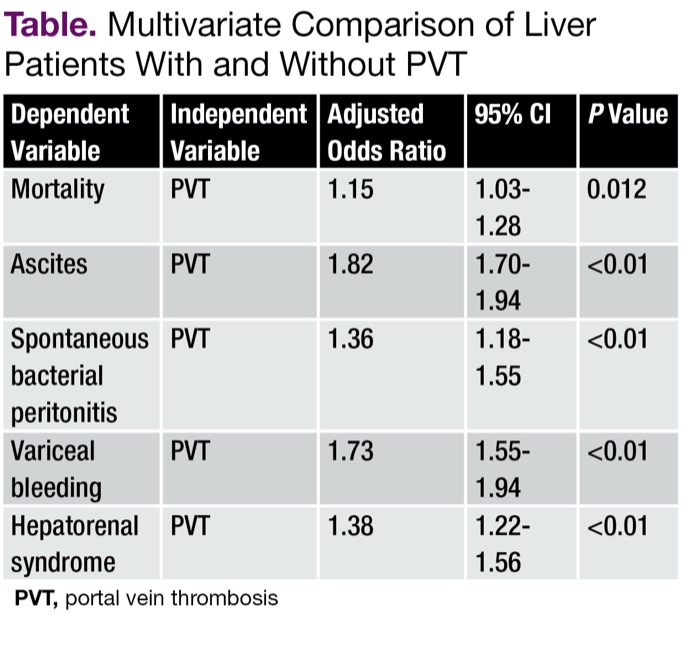
The 4,226 patients with PVT in the database were younger (61.9 vs. 62.5 years; P<0.01) and more likely to be men (79.8% vs. 75.6%; P<0.01) than those without the condition. Multivariate analyses controlling for age, sex, race, liver covariates and hepatic events confirmed the associations between PVT and hospital mortality, ascites and other complications (Table).
| Table. Multivariate Comparison of Liver Patients With and Without PVT | ||||
| Dependent Variable | Independent Variable | Adjusted Odds Ratio | 95% CI | P Value |
|---|---|---|---|---|
| Mortality | PVT | 1.15 | 1.03-1.28 | 0.012 |
| Ascites | PVT | 1.82 | 1.70-1.94 | <0.01 |
| Spontaneous bacterial peritonitis | PVT | 1.36 | 1.18-1.55 | <0.01 |
| Variceal bleeding | PVT | 1.73 | 1.55-1.94 | <0.01 |
| Hepatorenal syndrome | PVT | 1.38 | 1.22-1.56 | <0.01 |
| PVT, portal vein thrombosis | ||||
“As indicated by the odds ratios, the odds of adverse events were elevated between 10% to 90%,” Dr. Lee said.
Nancy Reau, MD, the section chief of hepatology at Rush Medical College in Chicago, said the findings effectively reinforce the need for early detection of PVT in hospitalized cirrhosis patients with primary liver cancer, but that providers should use caution when choosing the appropriate treatment.
“This study did not report anticoagulation use in the group with PVT and thus could not assess for the benefit of anticoagulation,” Dr. Reau said. “Given that there was a risk for variceal bleeding in those with PVT, anticoagulation must be used with trepidation.”
She added that patients with bland PVT may have different needs from those with tumor thrombosis. “This distinction is important for both prognosis as well as therapeutic options,” she said.
Dr. Lee agreed that more research is needed to better prognosticate outcomes and evaluate therapy options that will improve overall and disease-free survival.
—Adam Leitenberger
Drs. Lee and Reau reported no relevant financial disclosures.